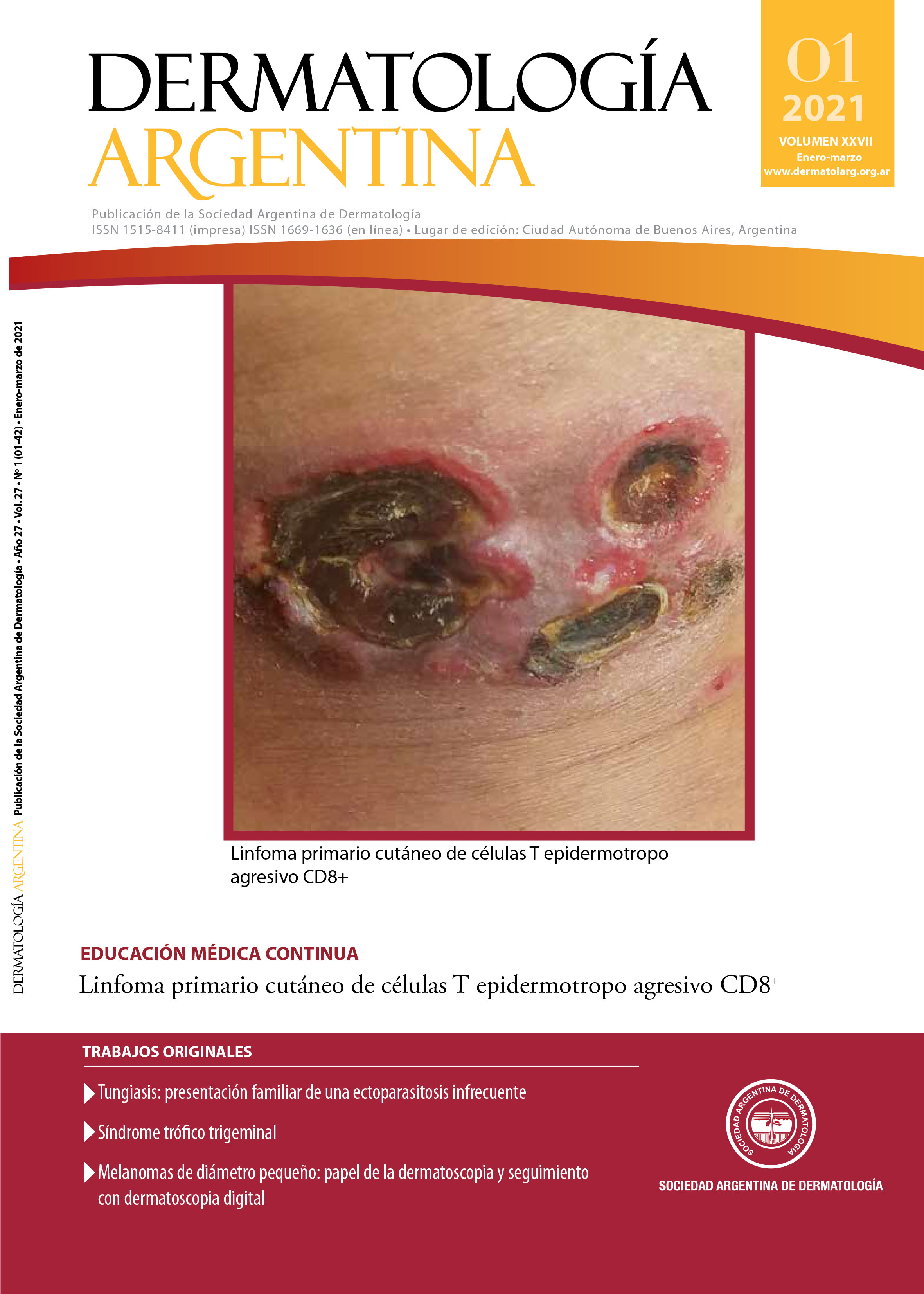
Linfoma primario cutáneo de células T epidermotropo agresivo CD8+
DOI:
https://doi.org/10.47196/da.v25i1.2194Palabras clave:
linfoma primario cutáneo, linfoma de Berti, epidermotropismoResumen
El linfoma de células T epidermotropo agresivo CD8+ o linfoma de Berti es un subtipo infrecuente de los linfomas primarios cutáneos, descripto en 1999. Aún se considera una entidad provisional en la última clasificación de linfomas cutáneos primarios de la Organización Mundial de la Salud. Predomina en los hombres adultos y se manifiesta con pápulas, placas hiperqueratósicas y tumores ulcerados, diseminados y de inicio agudo. En la histopatología, es característica la presencia de un infiltrado de linfocitos atípicos medianos CD8+, con epidermotropismo de patrón pagetoide. Tiene un comportamiento agresivo y es de mal pronóstico, con una sobrevida a los 5 años menor del 40%. Si bien esta entidad es un reto terapéutico, el tratamiento inicial se basa en poliquimioterapia y/o trasplante de células hematopoyéticas.
Referencias
I. Willemze R, Cerroni L, Kempf W, Berti E, et ál. The 2018 update of the WHO-EORTC classification for primary cutaneous lymphomas. Blood 2019;133:1703-1714.
II. Jensen J, Thestrup-Pedersen K. Subpopulations of T lymphocytes in a patient with fulminant mycosis fungoides. Acta Derm Venereol 1980;60:159-161.
III. Fujiwara Y, Abe Y, Kuyama M, Arata J, et ál. CD8+ Cutaneous T-cell lymphoma with pagetoid epidermotropism and angiocentric and angiodestructive infiltration. Arch Dermatol 1990;126:801-804.
IV. Urrutia S, Piris MA, Orradre JL, Martinez B, et ál. Cytotoxic/Suppressor (CD8+, CD4-) Cutaneous T-cell Lymphoma with Aggressive Course. Am J Dermatopathol 1990;12:603-606.
V. Agnarsson BA, Vonderheid EC, Kadin ME. Cutaneous T cell lymphoma with suppressor/cytotoxic (CD8) phenotype: Identification of rapidly progressive and chronic subtypes. J Am Acad Dermatol 1990;22:569-577.
VI. Sundram U. Cutaneous Lymphoproliferative Disorders: What’s New in the Revised 4th Edition of the World Health Organization (WHO) Classification of Lymphoid Neoplasms. Adv Anat Pathol 2019;26:93-113.
VII. Guitart J, Martinez-Escala ME, Subtil A, Duvic M, et ál. Primary cutaneous aggressive epidermotropic cytotoxic T-cell lymphomas: Reappraisal of a provisional entity in the 2016 WHO classification of cutaneous lymphomas. Mod Pathol 2017;30:761-772.
VIII. Robson A, Assaf C, Bagot M, Burg G, et ál. Aggressive epidermotropic cutaneous CD8+ lymphoma: A cutaneous lymphoma with distinct clinical and pathological features. Report of an EORTC Cutaneous Lymphoma Task Force Workshop. Histopathology 2015;67:425-441.
IX. Abeldaño A, Enz P, Maskin M, Cervini AB, et ál. Primary cutaneous lymphoma in Argentina: a report of a nationwide study of 416 patients. Int J Dermatol 2019;58:449-455.
X. El Shabrawi-Caelen L, Cerroni L, Kerl H. The clinicopathologic spectrum of cytotoxic lymphomas of the skin. Semin Cutan Med Surg 2000;19:118-123.
XI. Fanoni D, Corti L, Alberti-Violetti S, Tensen CP, et ál. Array-based CGH of primary cutaneous CD8+ aggressive EPIDERMO-tropic cytotoxic T-cell lymphoma. Genes Chromosom Cancer 2018;57:622-629.
XII. Willemze R. CD30-Negative cutaneous T-Cell lymphomas other than mycosis fungoides. Surg Pathol Clin 2014;7:229-252.
XIII. Nofal A, Abdel-Mawla MY, Assaf M, Salah E. Primary cutaneous aggressive epidermotropic CD8+ T-cell lymphoma: Proposed diagnostic criteria and therapeutic evaluation. J Am Acad Dermatol 2012;67:748-759.
XIV. Kempf W, Kazakov DV, Kerl K. Cutaneous lymphomas: An update. Part 1: T-cell and natural killer/T-Cell lymphomas and related conditions. Am J Dermatopathol 2014;36:105-123.
XV. Miyauchi T, Abe R, Morita Y, Adachi M, et ál. CD4/CD8 double-negative T-cell lymphoma: A variant of primary cutaneous CD8 + aggressive epidermotropic cytotoxic T-cell lymphoma? Acta Derm Venereol 2015;95:1024-1025.
XVI. Fierro MT, Novelli M, Savoia P, Cambieri I, et ál. CD45RA+ immunophenotype in mycosis fungoides: Clinical, histological and immunophenotypical features in 22 patients. J Cutan Pathol 2001;28:356-362.
XVII. Geller S, Myskowski PL, Pulitzer M, Horwitz SM, et ál. Cutaneous T-cell lymphoma (CTCL), rare subtypes: five case presentations and review of the literature. Chin Clin Oncol 2019;8:5.
XVIII. Jacks SM, Taylor BR, Rogers RP, Ralston JS, et ál. Rapid deterioration in a patient with primary aggressive cutaneous epidermotropic CD8+ cytotoxic T-cell ('Berti’) lymphoma after administration of adalimumab. J Am Acad Dermatol 2014;71:86-87.
XIX. Weenig RH, Comfere NI, Gibson LE, Alonso-Llamazares J, et ál. Fatal cytotoxic cutaneous lymphoma presenting as ulcerative psoriasis. Arch Dermatol 2009;145:801-808.
XX. Wang Y, Li T, Tu P, Wu LS, et ál. Primary cutaneous aggressive epidermotropic CD8+ cytotoxic T-cell lymphoma clinically simulating pyoderma gangrenosum. Clin Exp Dermatol 2009;34:261-262.
XXI. Deenen NJ, Koens L, Jaspars EH, Vermeer MH, et ál. Pitfalls in diagnosing primary cutaneous aggressive epidermotropic CD8 + T-cell lymphoma. Br J Dermatol 2019;180:411-412.
XXII. Tomasini C, Novelli M, Fanoni D, Berti EF. Erythema multiforme-like lesions in primary cutaneous aggressive cytotoxic epidermotropic CD8+ T-cell lymphoma: a diagnostic and therapeutic challenge. J Cutan Pathol 2017;44:867-873.
XXIII. Martinez-Escala ME, Kantor RW, Cices A, Zhou XA, et ál. CD8+ mycosis fungoides: a low-grade lymphoproliferative disorder. J Am Dermatology 2017;77:489-496.
XXIV. Haghighi B, Smoller BR, LeBoit PE, Warnke RA, et ál. Pagetoid reticulosis (Woringer-Kolopp disease): An immunophenotypic, molecular, and clinicopathologic study. Mod Pathol 2000;13:502-510.
XXV. Mourtzinos N, Puri PK, Wang G, Liu ML. CD4/CD8 double negative pagetoid reticulosis: a case report and literature review. J Cutan Pathol 2010 Apr;37(4):491-6.
XXVI. Ally MS, Robson A. A review of the solitary cutaneous T-cell lymphomas. J Cutan Pathol 2014;41:703-714.
XXVII. Marschalkó M, Gyöngyösi N, Noll J, Károlyi Z, et ál. Histopathological aspects and differential diagnosis of CD8 positive lymphomatoid papulosis. J Cutan Pathol 2016;43:963-973.
XXVIII. Saggini A, Gulia A, Argenyi Z, Fink-Puches R, et ál. A variant of lymphomatoid papulosis simulating primary cutaneous aggressive epidermotropic CD8+ cytotoxic T-cell lymphoma. Description of 9 cases. Am J Surg Pathol 2010;34:1168-1175.
XXIX. Martires KJ, Ra S, Abdulla F, Cassarino DS. Characterization of primary cutaneous CD8+/CD30+ lymphoproliferative disorders. Am J Dermatopathol 2015;37:822-833.
XXX. Plaza JA, Feldman AL, Magro C. Cutaneous CD30-positive lymphoproliferative disorders with CD8 expression: A clinicopathologic study of 21 cases. J Cutan Pathol 2013;40:236-247.
XXXI. Magro CM, Crowson AN, Morrison C, Merati K, et ál. CD8+ lymphomatoid papulosis and its differential diagnosis. Am J Clin Pathol 2006;125:490-501.
XXXII. McQuitty E, Curry JL, Tetzlaff MT, Prieto VG, et ál. The differential diagnosis of CD8-positive (‘type D’) lymphomatoid papulosis. J Cutan Pathol 2014;41:88-100.
XXXIII. Wieser I, Tetzlaff MT, Torres Cabala CA, Duvic M. Primary Cutaneous CD30+ Lymphoproliferative Disorders. J Dtsch Dermatol Ges 2016;14:767-782.
XXXIV. Baldin P, Shwe MM, Marot L, Eeckout PVV, Dachelet C, Sacré L, Berners A, Olivier S, Camboni A. Primary cutaneous CD8+ and CD30+ T-cell lymphoproliferative disorders: case reports and clinical implications. Eur J Dermatol 2019;29(1):39-44.
XXXV. Quintanilla-Martinez L, Jansen PM, Kinney MC, Swerdlow SH, et ál. Non-mycosis fungoides cutaneous T-cell lymphomas report of the 2011 society for hematopathology/European association for haematopathology workshop. Am J Clin Pathol 2013;139:491-514.
XXXVI. Petrella T, Maubec E, Cornillet-Lefebvre P, Willemze R, et ál. Indolent CD8-positive lymphoid proliferation of the ear: A distinct primary cutaneous T-cell lymphoma? Am J Surg Pathol 2007;31:1887-1892.
XXXVII. Li JY, Guitart J, Pulitzer MP, Subtil A, et ál. Multicenter case series of indolent small/medium-sized CD8+ lymphoid proliferations with predilection for the ear and face. Am J Dermatopathol 2014;36:402-408.
XXXVIII. Wobser M, Roth S, Reinartz T, Rosenwald A, et ál. CD68 expression is a discriminative feature of indolent cutaneous CD8-positive lymphoid proliferation and distinguishes this lymphoma subtype from other CD8-positive cutaneous lymphomas. Br J Dermatol 2015;172:1573-1580.
XXXIX. Cocks M, Porcu P, Wick MR, Gru AA. Recent advances in cutaneous T-cell lymphoma: diagnostic and pronostic considerations. Surg Pathol 2017;12: 83-803.
XL. Toro JR, Beaty M, Sorbara L, Turner ML, et ál. γδ T-cell lymphoma of the skin: A clinical, microscopic, and molecular study. Arch Dermatol 2000;136:1024-1032.
XLI. Guitart J, Weisenburger DD, Subtil A, Kim E, et ál. Cutaneous γδ T-cell Lymphomas: a spectrum of presentations with overlap with other citotoxic lymphomas. Am J Surg Pathol 2012;36:1656-1665.
XLII. Geller S, Myskowski PL, Pulitzer M. NK/T-cell lymphoma, nasal type, γδ T-cell lymphoma, and CD8-positive epidermotropic T-cell lymphoma- clinical and histopathologic features, differential diagnosis, and treatment. Semin Cutan Med Surg 2018;37:30-38.
XLIII. Kim YH, Willemze R, Pimpinelli N, Whittaker S, et ál. TNM classification system for primary cutaneous lymphomas other than mycosis fungoides and Sézary syndrome: a proposal of the International Society fot Cutaneous Lymphomas (ISCL) and the Cutaneous Lymphoma Task Force of the European Organization of Research and Treatment of Cancer (EORTC). Blood 2007;110:479-484.
XLIV. Gormley RH, Hess SD, Anand D, Junkins-Hopkins J, et ál. Primary cutaneous aggressive epidermotropic CD8+ T-cell lymphoma. J Am Acad Dermatol 2010;62:300-307.
XLV. Introcaso CE, Kim EJ, Gardner J, Junkins-Hopkins JM, et ál. CD8+ epidermotropic cytotoxic T-cell lymphoma with peripheral blood and central nervous system involvement. Arch Dermatol 2008;144:1027-1029.
XLVI. Marzano A V, Ghislanzoni M, Gianelli U, Caputo R, et ál. Fatal CD8+ epidermotropic cytotoxic primary cutaneous T-cell lymphoma with multiorgan involvement. Dermatology 2005;211:281-85.
XLVII. Berti E, Tomasini D, Vermeer MH, Meijer CJ, et ál. Primary cutaneous CD8-positive epidermotropic cytotoxic T cell lymphomas. Am J Pathol 1999;155:483-92.
XLVIII. Wobser M, Reinartz T, Roth S, Goebeler M, et ál. Cutaneous CD8+ Cytotoxic T-Cell Lymphoma Infiltrates: Clinicopathological Correlation and Outcome of 35 Cases. Oncol Ther 2016;4:199-210.
XLIX. Nofal A, Abdel-Mawla MY, Assaf M, Salah E, et ál. Primary cutaneous aggressive epidermotropic CD8+ T cell lymphoma: A diagnostic and therapeutic challenge. Int J Dermatol 2014;53:76-81.
L. Santucci M, Pimpinelli N, Massi D, Kadin ME, et ál. Cytotoxic/natural killer cell cutaneous lymphomas: Report of the EORTC Cutaneous Lymphoma Task Force workshop. Cancer 2003;97:610-627.
LI. Liu V, Cutler CS, Young AZ. Case records of the Massachusetts General Hospital Case 38-2007. A 44-year-old woman with generalized, painful, ulcerated skin lesions. N Engl J Med 2007;357:2496-2505.
LII. Csomor J, Bognár Á, Benedek S, Sinkó J, et ál. Rare provisional entity: Primary cutaneous aggressive epidermotropic CD8+ cytotoxic T-cell lymphoma in a young woman. J Clin Pathol 2008;61:770-772.
LIII. Intriago BM, Peña OC, Gray HA, Cabrera CM, et ál. Linfoma primario cutáneo agresivo epidermotrópico de células T citotóxicas CD8 positivo. Caso clínico. Rev Med Chil 2012;140:368-372.
LIV. Wehkamp U, Glaeser D, Oschlies I, Hilgendorf I, et ál. Successful stem cell transplantation in a patient with primary cutaneous aggressive cytotoxic epidermotropic CD8 + T-cell lymphoma. Br J Dermatol 2015;173:869-871.
LV. Saruta H, Ohata C, Oku E, Natsuaki Y, et ál. Successful autologous peripheral blood stem cell transplantation in primary cutaneous aggressive epidermotropic CD8+ T-cell lymphoma. J Dtsch Dermatol Ges 2017;15:440-442.
LVI. Cyrenne BM, Gibson JF, Subtil A, Girardi M, et ál. Transplantation in the Treatment of Primary Cutaneous Aggressive Epidermotropic Cytotoxic CD8-Positive T-Cell Lymphoma. Clin Lymphoma, Myeloma Leuk 2018;18:85-93.
LVII. Yoshizawa N, Yagi H, Horibe T, Takigawa M, et ál. Primary cutaneous aggressive epidermotropic CD8+ T-cell lymphoma with a CD15+ CD30– phenotype. Eur J Dermatol 2007;17:441-442.
LVIII. Webber NK, Harwood C, Goldsmith P, Cerio R, et ál. Aggressive epidermotropic cutaneous CD8+ (Berti’s) lymphoma: CPD. A memorable patient. Clin Exp Dermatol 2010;35:210-212.
LIX. Brüggen MC, Kerl K, Haralambieva E, Schanz U, et ál. Aggressive rare T-cell lymphomas with manifestation in the skin: A monocentric cross-sectional case study. Acta Derm Venereol 2018;98:835-841.
LX. Kerdel FA, Styperek AR, Maini A. Clinical remission of primary aggressive CD8+ cutaneous T-cell lymphoma after pralatrexate infusion. JAMA Dermatology 2014;150:320-322.
LXI. Cyrenne BM, Subtil A, Girardi M, Foss F. Primary cutaneous aggressive epidermotropic cytotoxic CD8 + T-cell lymphoma: long-term remission after brentuximab vedotin. Int J Dermatol 2017;56:1448-1450.
LXII. Moskowitz AJ, Horwitz SM. Targeting histone deacetylases in T-cell lymphoma. Leuk Lymphoma 2017;58:1306-1319.
Descargas
Publicado
Número
Sección
Licencia
El/los autor/es tranfieren todos los derechos de autor del manuscrito arriba mencionado a Dermatología Argentina en el caso de que el trabajo sea publicado. El/los autor/es declaran que el artículo es original, que no infringe ningún derecho de propiedad intelectual u otros derechos de terceros, que no se encuentra bajo consideración de otra revista y que no ha sido previamente publicado.
Le solicitamos haga click aquí para imprimir, firmar y enviar por correo postal la transferencia de los derechos de autor